



HIV stands for human immunodeficiency virus. It is the virus that can lead to acquired immunodeficiency syndrome, or AIDS. Unlike some other viruses, the human body cannot get rid of HIV. That means that once you have HIV, you have it for life.
No safe and effective cure currently exists, but scientists are working hard to find one, and remain hopeful. Meanwhile, with proper medical care, HIV can be controlled. Treatment for HIV is often called antiretroviral therapy or ART. It can dramatically prolong the lives of many people infected with HIV and lower their chance of infecting others. Before the introduction of ART in the mid-1990s, people with HIV could progress to AIDS in just a few years. Today, someone diagnosed with HIV and treated before the disease is far advanced can have a nearly normal life expectancy.
HIV affects specific cells of the immune system, called CD4 cells, or T cells. Over time, HIV can destroy so many of these cells that the body can’t fight off infections and disease. When this happens, HIV infection leads to AIDS.
The only way to know if you are infected with HIV is to be tested. You cannot rely on symptoms to know whether you have HIV. Many people who are infected with HIV do not have any symptoms at all for 10 years or more. Some people who are infected with HIV report having flu-like symptoms (often described as “the worst flu ever”) 2 to 4 weeks after exposure. Symptoms can include:
Fever
Enlarged lymph nodes
Sore throat
Rash
These symptoms can last anywhere from a few days to several weeks. During this time, HIV infection may not show up on an HIV test, but people who have it are highly infectious and can spread the infection to others.
However, you should not assume you have HIV if you have any of these symptoms. Each of these symptoms can be caused by other illnesses. Again, the only way to determine whether you are infected is to be tested for HIV infection.
Getting an HIV test is the only way to know if you have HIV.
The most common HIV test is the antibody screening test (immunoassay), which tests for the antibodies that your body makes against HIV. The immunoassay may be conducted in a lab or as a rapid test at the testing site. It may be performed on blood or oral fluid (not saliva). Because the level of antibody in oral fluid is lower than it is in blood, blood tests tend to find infection sooner after exposure than do oral fluid tests. In addition, most blood-based lab tests find infection sooner after exposure than rapid HIV tests.
Several tests are being used more commonly that can detect both antibodies and antigen (part of the virus itself). These tests can find recent infection earlier than tests that detect only antibodies. These antigen/antibody combination tests can find HIV as soon as 3 weeks after exposure to the virus, but they are only available for testing blood, not oral fluid.
The rapid test is an immunoassay used for screening, and it produces quick results, in 30 minutes or less. Rapid tests use blood or oral fluid to look for antibodies to HIV. If an immunoassay (lab test or rapid test) is conducted during the window period (i.e., the period after exposure but before the test can find antibodies), the test may not find antibodies and may give a false-negative result. All immunoassays that are positive need a follow-up test to confirm the result.
Follow-up diagnostic testing is performed if the first immunoassay result is positive. Follow-up tests include: an antibody differentiation test, which distinguishes HIV-1 from HIV-2; an HIV-1 nucleic acid test, which looks for virus directly, or the Western blot or indirect immunofluorescence assay, which detect antibodies.
Immunoassays are generally very accurate, but follow-up testing allows you and your health care provider to be sure the diagnosis is right. If your first test is a rapid test, and it is positive, you will be directed to a medical setting to get follow-up testing. If your first test is a lab test, and it is positive, the lab will conduct follow-up testing, usually on the same blood specimen as the first test.
Currently there are only two home HIV tests: the Home Access HIV-1 Test System and the OraQuick In-home HIV test. If you buy your home test online make sure the HIV test is FDA-approved.
The Home Access HIV-1 Test System is a home collection kit, which involves pricking your finger to collect a blood sample, sending the sample to a licensed laboratory, and then calling in for results as early as the next business day. This test is anonymous. If the test is positive, a follow-up test is performed right away, and the results include the follow-up test. The manufacturer provides confidential counseling and referral to treatment. The tests conducted on the blood sample collected at home find infection later after infection than most lab-based tests using blood from a vein, but earlier than tests conducted with oral fluid.
The OraQuick In-Home HIV Test provides rapid results in the home. The testing procedure involves swabbing your mouth for an oral fluid sample and using a kit to test it. Results are available in 20 minutes. If you test positive, you will need a follow-up test. The manufacturer provides confidential counseling and referral to follow-up testing sites. Because the level of antibody in oral fluid is lower than it is in blood, oral fluid tests find infection later after exposure than do blood tests. Up to 1 in 12 people may test false-negative with this test.
RNA tests detect the virus directly (instead of the antibodies to HIV) and thus can detect HIV at about 10 days after infection—as soon as it appears in the bloodstream, before antibodies develop. These tests cost more than antibody tests and are generally not used as a screening test, although your doctor may order one as a follow-up test, after a positive antibody test, or as part of a clinical workup.
Once you receive a diagnosis of HIV, the most important next step is to get into medical care. Getting into medical care and staying on treatment will help you manage your HIV effectively and make decisions that can keep you healthy for many years.
Pay attention to your mental health. Receiving a diagnosis of HIV can be a life-changing event. People can feel many emotions – sadness, hopelessness, and even anger. But having HIV is by no means a death sentence. Allied health care providers and social service providers, often available at your health care provider’s office, will have the tools to help you work through the early stages of your diagnosis and begin to manage your HIV.
Talking to others who have HIV may also be helpful. Find a local HIV support group. Learning about how other people living with HIV have handled their diagnosis may be helpful.
You can live well with HIV. Many resources and support programs are available to help you make decisions and take actions to live a longer and healthier life. Understanding certain terms—like HIV, AIDS, and antiretroviral therapy (ART)—will help you take the first steps in managing your HIV.
The drugs commonly used to treat HIV are called antiretroviral therapy (ART). ART is recommended for all people with HIV, regardless of how long they’ve had the virus or how healthy they are. If you have HIV it is important that you get in care and start ART right away.
For people with HIV, ART reduces the amount of virus in the blood and elsewhere in the body. The amount of virus is called the “viral load.” When we measure the amount of virus in blood, we measure it in the part of blood called “plasma” and refer to this amount of virus as the “plasma viral load.”
ART is extremely effective and can reduce the level of HIV in the blood to such a low level that current HIV tests cannot detect it. This is called “undetectable viral load.” The goal of ART is to reduce viral load, ideally to an undetectable level. If a person’s viral load goes down after starting ART, then the treatment is working. ART can keep you healthy for many years, and greatly reduce your chance of transmitting HIV to partners if taken consistently and correctly.
ART usually consists of a combination of medicines that needs to be taken exactly as your health care provider prescribes. How many pills you need and how often you take them will depend on which medicines you and your health care provider select.
There is no one “best” treatment for HIV. You and your health care provider may decide to change your treatment plan to fit your health care needs and life situation, which may change over time.
Today, more tools than ever are available to prevent HIV. In addition to limiting your number of sexual partners, never sharing needles, and using condoms correctly and consistently, you may be able to take advantage of newer biomedical options such as pre-exposure and post-exposure prophylaxis.
Choose less risky sexual behaviors, limit your number of sex partners, use condoms, use medicines to prevent HIV if appropriate, and get checked for sexually transmitted diseases (STDs).
Avoid having your partner ejaculate in your mouth, and use barriers such as condoms, natural rubber latex sheets, dental dams, or cut-open non-lubricated condoms between your mouth and your partners’ genitals.
When used correctly and consistently, condoms are highly effective in preventing HIV infection. Water-based and silicon-based lubricants are safe to use with latex condoms. Oil-based lubricants and products containing oil, such as hand lotion, Vaseline, or Crisco should not be used with latex condoms. It is safe to use any kind of lubricant with nitrile female condoms.
Male circumcision reduces the risk that a man will get HIV from an infected female partner, and also lowers the risk of other sexually transmitted infections (STIs), penile cancer, and infant urinary tract infection. Studies have not consistently shown that it prevents HIV among men who have sex with men. Circumcision is only partly effective and should be used with other prevention measures. Men who are considering circumcision should weigh its risks and costs against its potential benefits.
Pre-exposure prophylaxis, or PrEP, can lower the risk of getting HIV by taking a pill every day. It is for people who do not have HIV but who are at substantial risk of getting it.
Post-exposure prophylaxis (PEP) is medicine that can prevent HIV after a possible exposure if started within 3 days.

HIV/AIDS 101

HIV Treatment as Prevention

Youth Behaviors and HIV Risk

HIV Prevention

HIV/TB Co-Infection

CDC: Dena's Story, Let's Stop HIV Together
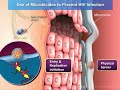
Transmission and Prevention of HIV

CDC: Masonia's Story, Let's Stop HIV Together

CDC: JJ's Story, Let's Stop HIV Together

Swizz Beatz Urges Young People to Act Against AIDS

CDC: Michelle's Story, Let's Stop HIV Together

STI screening as HIV prevention

HIV: The Goal of Undetectable (USA)

HIV: What's Going on Inside Your Body (USA)

HIV: Help Stop the Virus (USA)

A study suggests that breastfeeding may help women with a history of gestational diabetes from...

About 1 in 3 adults in the U.S. has high blood pressure, but many don’t realize it. High...

We make dozens of decisions every day. When it comes to deciding what to eat and feed our...

Do you tend to look on the sunny side, or do you see a future filled with dark, stormy skies?...